Skin pigmentation disorders fall into two main categories: hypopigmentation and hyperpigmentation. Hypopigmentation refers to skin areas that are lighter than a person’s natural skin tone, while hyperpigmentation occurs when skin patches become darker. Some women may develop hyperpigmentation during menopause, including a condition called melasma. Melasma is a common skin disorder in which tan, brown, or blue-gray patches and spots develop symmetrically on the face or other areas of the body regularly exposed to sunlight.(1)
Melasma most often affects women with medium to dark skin tones. The condition is not cancerous or contagious and has been linked to a number of contributing factors, including hormonal changes.(2) This article will explore how skin pigmentation may change throughout perimenopause and menopause and how women can manage melasma and hyperpigmentation as they age.
Understanding Melasma and Hyperpigmentation in Menopause
Menopause is a life event marked by fluctuations in hormone levels, including estrogen and progesterone. Estrogen influences the activity of skin cells called melanocytes. These cells contain melanin, a substance that produces pigment in the eyes, hair, and skin. Melanin protects the cells against damage from ultraviolet (UV) radiation — a process known to be influenced by estrogen and progesterone. Greater amounts of melanin in the body can lead to hyperpigmentation and melasma.(1)(3)
Women in the later stages of pregnancy are also prone to melasma, further illustrating an association between hormonal changes and hyperpigmentation. The condition has also been linked to the use of oral contraceptive pills. Hormonal shifts during menopause may also cause changes in skin pigmentation.(4)
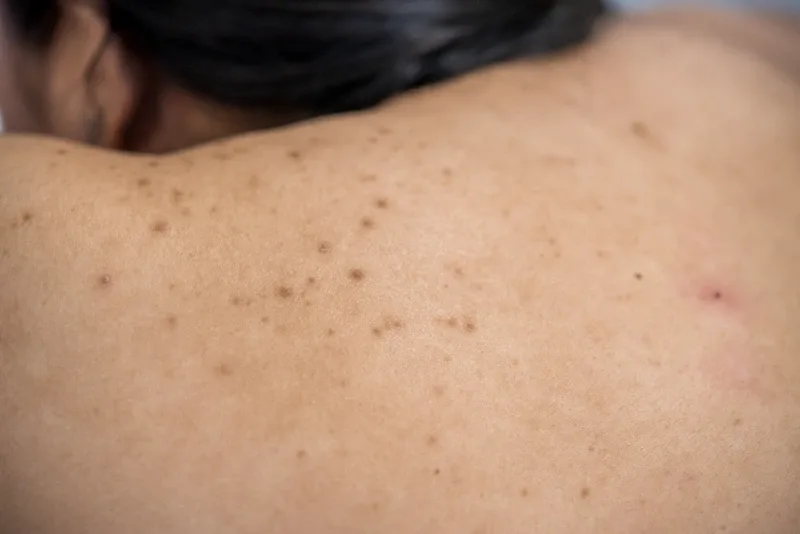
Symptoms of menopause-related melasma may manifest differently in the body. Melasma commonly affects the face. However, extrafacial melasma — characterized by darker skin patches on areas such as the forearms, back, or chest — is more frequently observed in postmenopausal women. In fact, as many as 80% of women with extrafacial melasma are postmenopausal.(5)
Because the number of melanocytes in the body decreases with age, not all women may experience skin hyperpigmentation during this phase of life. Additionally, while research indicates a relationship between estrogen and melasma, some studies suggest that this connection may not extend to menopause.(5)
Causes of Menopause-Related Hyperpigmentation and Melasma
It’s not clear what causes melasma. However, in addition to hormone changes, there are other factors that may contribute to hyperpigmentation or melasma that develops during menopause, including the following:(1)(3)(6)
UV Ray Exposure: Sun exposure is a major risk factor for melasma and hyperpigmentation. When the skin is exposed to sunlight, the body increases melanin production to protect against UV rays. This process involves boosting the activity of certain enzymes that trigger a series of chemical reactions to produce more pigment. However, without proper protection, chronic UV ray exposure can lead to cell damage caused by free radicals.
Genetics: A person may be more prone to developing melasma if they have a family member with the condition. Melasma may also be influenced by changes in DNA.
Medication Use: Certain drugs can cause hyperpigmentation, especially those that increase photosensitivity. In addition to birth control pills, medications such as antibiotics, corticosteroids, and retinoids can trigger the condition.
Hormone Replacement Therapy (HRT): Hyperpigmentation is a potential side effect of HRT. Some studies suggest a link between HRT and extrafacial melasma in menopausal women, particularly on the arms.
Stress Levels: Stress raises cortisol levels, which may play a role in the development of melasma.
Inflammation: Post-inflammatory hyperpigmentation can occur as a result of physical trauma, eczema, or other forms of skin inflammation.
Health Conditions: Certain health conditions that affect hormone-producing organs in the body, such as thyroid disorders or ovarian tumors, may impact skin pigmentation.
How does perimenopause affect skin pigmentation changes?
Most women begin experiencing perimenopausal symptoms between the ages of 45 and 55; these symptoms may include changes in skin pigmentation as hormone levels start to fluctuate. Women entering the menopause transition may be more likely to experience specific types of skin pigmentation disorders. For example, cases of acquired bilateral melanosis (ABM) have been documented in perimenopausal women, in which brown or gray patches of skin or blotchy skin develop on both sides of the neck. The exact cause of ABM is not well understood.(5)(7)
Poikiloderma of Civatte (PC) is another skin pigmentation disorder characterized by pink or brown patches of skin on the face, neck, and chest. The condition typically affects people with lighter skin tones and is often seen in perimenopausal women. Like melasma, it’s believed to be influenced by genetics, UV ray exposure, and estrogen loss.(5)(8)
Treatment and Prevention of Menopause Hyperpigmentation
A dermatologist will use specialized medical tools to examine a patient's skin and diagnose melasma. They may also recommend a skin biopsy to rule out other skin conditions. In some cases, melasma may naturally fade over time, such as following childbirth or after discontinuing certain medications. However, for others, hyperpigmentation may persist indefinitely.(9)
Treatment plans will vary depending on the skin tone and how deeply hyperpigmentation has penetrated the skin. In general, a doctor may recommend the following prevention or treatment methods:(9)
UV Ray Protection: Daily application of a broad-spectrum SPF 30+ sunscreen can protect against melasma and prevent existing hyperpigmentation from worsening. While melasma may fade in the winter, sun protection is particularly important during the summer months when skin is more exposed to UV rays. Sunscreen products containing zinc oxide, iron oxide, or titanium dioxide may specifically be recommended. Tanning beds pose the same risks as sun exposure and should also be avoided.
Topical or Oral Medications: Hydroquinone is a topical prescription medication frequently used to treat melasma. Other topical treatments may include a combination of tretinoin and an anti-inflammatory corticosteroid. In some cases, all three medications may simultaneously be prescribed. A doctor may also recommend products containing azelaic acid or vitamin C. Oral or topical tranexamic acid may be prescribed for more severe cases of melasma.
Skin Procedures: Laser therapy, microneedling, chemical peels, or platelet-rich plasma procedures are treatment options that may be recommended alongside medication use. These procedures can help reduce pigmentation and even out skin tone.
Medications and skin procedures can have side effects, including peeling or skin irritation. Women should speak with their dermatologist about the benefits and risks of different melasma treatment methods. While melasma can recur, many patients see improvement in their skin’s appearance with professional treatment.(3)(4)
Practical Tips for Managing Menopause Skin Pigmentation Changes
It can take anywhere from three months to one year to see improvement in hyperpigmentation. The following are ways women can manage skin pigmentation changes during menopause while undergoing professional treatment:(1)(9)(10)
Using Cosmetic Products: Camouflage makeup products contain pigments that can help mask discoloration and blemishes. Makeup should be used only after treatment medication and sunscreen have been applied to the skin.
Maintaining a Gentle Skincare Routine: Cleansing and moisturizing the skin twice a day with products free of irritating ingredients can help keep the skin healthy and bright.
Eating a Diet Rich in Omega-3s: Omega-3 fatty acids may help reduce inflammation. A study published in the Journal of the American Academy of Dermatology found that omega-3 supplements may help reduce post-inflammatory skin hyperpigmentation in patients following laser therapy treatment.
Trying Natural Supplements: Research on the safety and health benefits of supplements is limited. However, some studies suggest that certain vitamins and herbal remedies may help improve hyperpigmentation. Niacin and biotin are B vitamins that can be found in many over-the-counter (OTC) products designed to improve the skin’s appearance. Aloe vera, argan oil, turmeric extract, and green tea extract may also help reduce hyperpigmentation. Individuals should consult with their healthcare provider before taking any new medications or supplements.
Embracing Skin Pigmentation Changes During Menopause
Skin changes are often viewed as an aesthetic problem, which can create barriers to treatment for patients. Changes in skin pigmentation can affect women’s mental, emotional, and social well-being. However, these changes can be effectively managed with a personalized treatment plan.
Skin changes are common during menopause. Along with hyperpigmentation, women may notice fine lines, wrinkles, and reduced elasticity as the skin loses collagen and moisture with age. With self-care, a healthy skincare regimen, and support from a dermatologist, women can embrace the menopause-related skin changes that naturally accompany this phase of life.
